What is rosacea?
Rosacea, also known as a facial redness disorder, is a common and chronic skin condition that causes persistent redness, sensitivity, and sometimes acne-like bumps. Although it usually appears on the central areas of the face—particularly the cheeks and nose—it can still be managed effectively with the right approach. Moreover, many people notice that their symptoms change over time, yet a consistent routine often helps the skin stay calmer and more balanced.
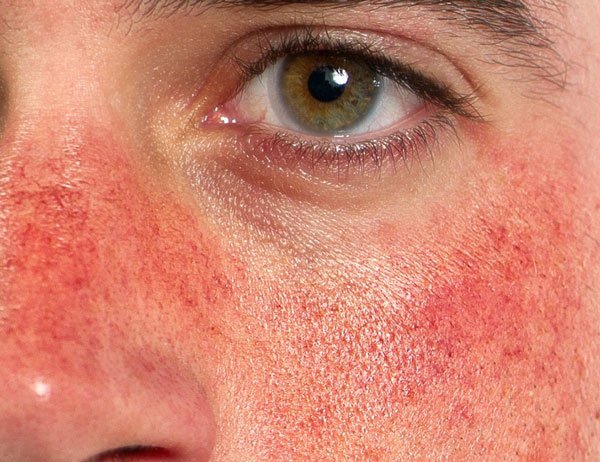
Causes and triggers of rosacea
The exact cause of this redness disorder is not yet fully understood. However, research suggests that genetics, inflammation, vascular sensitivity, and environmental factors all play a role. Additionally, many individuals live with persistent redness for years before realising that their symptoms are related to this condition.
Common rosacea triggers
Understanding what aggravates the skin is often the first step toward better control. While triggers vary from person to person, several are widely recognised.
Emotional triggers
Stress, anxiety, embarrassment, and strong emotions may lead to facial flushing. Although this response is natural, learning stress-management techniques can help minimise flare-ups.
Weather conditions
Environmental changes—from cold winds to intense heat—often worsen rosacea flares. Moreover, sun exposure is one of the most common triggers. UV light dilates blood vessels and increases heat in the skin, which intensifies redness.
Lifestyle factors
Daily habits may also influence rosacea symptoms. These include:
- Spicy foods
- Hot drinks
- Alcohol (especially red wine)
- Intense exercise
- Certain medications
Because each person reacts differently, keeping a personal trigger diary can be extremely helpful.
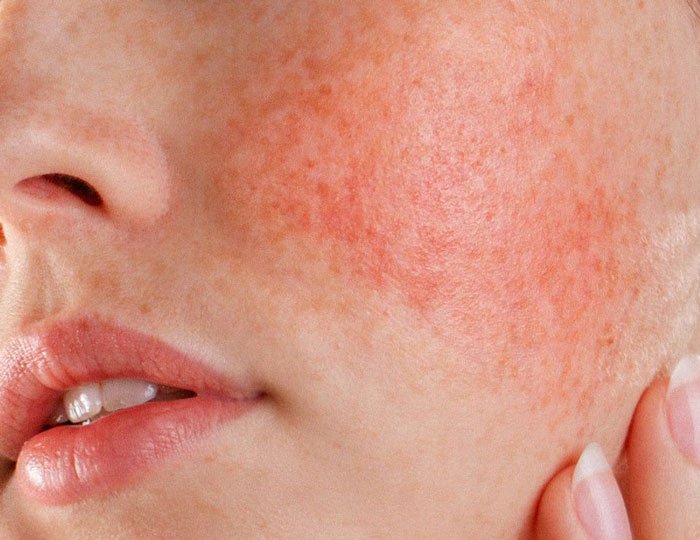
Types of rosacea
Identifying the subtype of rosacea supports more effective treatment decisions. While some individuals may experience a combination of types, the most common categories include:
Erythematotelangiectatic rosacea (ETR)
Characterised by persistent redness, visible capillaries, and sensitivity.
Papulopustular rosacea
Includes red bumps and occasional pus-filled lesions, resembling acne.
Phymatous rosacea
Causes skin thickening, often around the nose (rhinophyma).
Ocular rosacea
Affects the eyes, leading to irritation, burning, and redness.

Rosacea treatment options
Although this condition has no permanent cure, its symptoms can improve significantly with consistent care and targeted treatments. Importantly, combining clinical treatments with gentle daily habits often offers the best results.
Topical treatments
Products such as azelaic acid or metronidazole can reduce inflammation and improve mild rosacea over several weeks.
Oral medications
For moderate to severe cases, anti-inflammatory oral antibiotics may be prescribed to calm deeper inflammation.
Laser & light-based treatments for rosacea
Light-based therapies—including IPL and laser skin rejuvenation—are among the most effective options for reducing persistent redness and visible capillaries. These technologies heat targeted blood vessels to minimise their appearance while also stimulating collagen for a smoother, more even complexion.
Chemical peels
Gentle chemical peels may support barrier repair and reduce surface inflammation in suitable skin types.
HydraFacial
When customised appropriately, HydraFacial can help hydrate, soothe, and balance sensitive rosacea-prone skin.
Lifestyle adjustments
Alongside clinical methods, avoiding known triggers—such as extreme temperatures, spicy foods, and alcohol—plays an essential role in maintaining stable skin
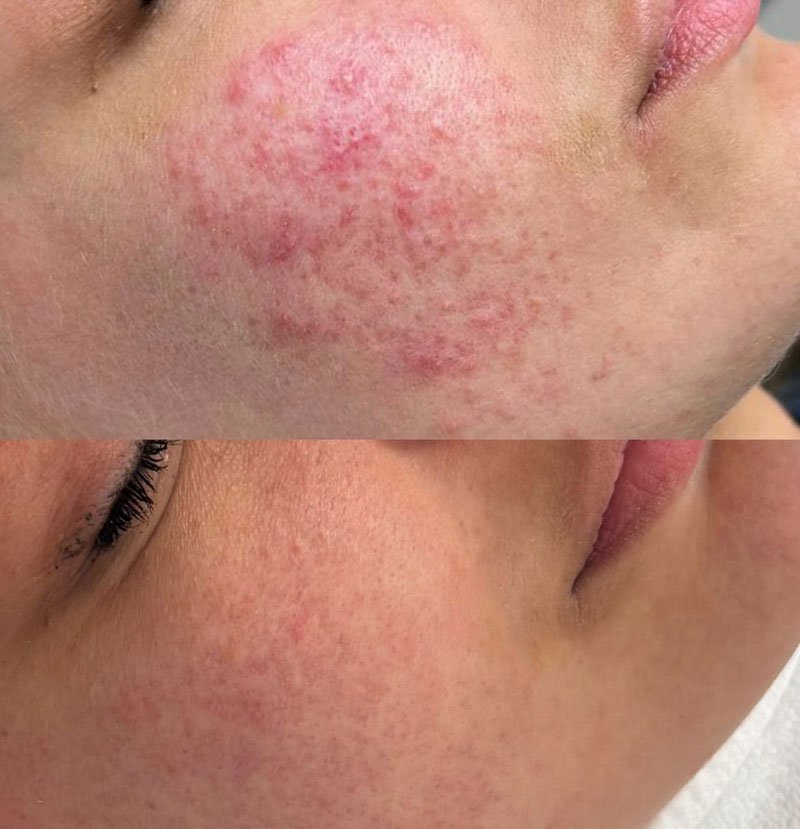
How Medix can help
After reviewing available options, choosing an experienced clinic can make managing this concern becomes easier. At Medix Skin & Laser Clinic, every treatment plan is personalised based on your skin type, sensitivity pattern, flare triggers, and long-term goals.
Furthermore, Medix offers modern, non-invasive treatments such as:
- Laser Skin Rejuvenation
- Pigmentation Removal
- Radiofrequency Skin Needling
- HydraFacial
- Chemical Peels
These techniques are selected thoughtfully to reduce redness, strengthen the skin barrier, and help the complexion become more comfortable and even over time.
Service reservation
Book a consultation today, and together we’ll create a personalised plan to calm redness, strengthen your skin, and help you feel more comfortable and confident in your complexion.
Contact Medix Clinic
For more information, feel free to contact us at 03 9686 0003.
You can also visit our clinic at 1/367A Centre Road, Bentleigh, Victoria 3204.
Click here to view our location on Google Maps.
About Medix Skincare and Laser Clinic in Melbourne
In the end, managing this concern is a journey—yet you don’t have to navigate it alone. Once you understand your triggers and learn how your skin responds, meaningful improvements begin to appear.
If you’re ready to experience calmer, clearer, and more confident skin, a consultation at Medix can be a reassuring first step. During this session, your skin will be assessed thoroughly, and a personalised treatment plan will be created to support your unique needs.
Book a consultation today and take the next gentle step toward healthier, more balanced skin.
Frequently Asked Questions
Although triggers vary from person to person, several factors commonly increase redness—such as sun exposure, emotional stress, hot drinks, spicy foods, and sudden temperature changes. Fortunately, once you identify your personal triggers, managing flare-ups becomes much easier.
While rosacea is a long-term condition, its symptoms can improve significantly with consistent care and the right lifestyle adjustments. In many cases, simple habits—like daily sunscreen, gentle skincare, and avoiding triggers—help the skin stay calmer over time.
Several evidence-based options can support this concern. For example, IPL, laser rejuvenation, chemical peels, and HydraFacial can all reduce redness and strengthen the skin barrier when selected properly. As a result, many people notice smoother and more even-toned skin after a series of tailored treatments
Not exactly. Although both may include bumps or inflammation, rosacea is primarily a vascular and sensitivity-related condition. However, the good news is that with the right plan, both redness and acne-like flare-ups can be managed safely and effectively.
A gentle routine makes a big difference. Using a mineral sunscreen, choosing mild cleansers, avoiding excessive heat, and moisturising regularly can help your skin stay balanced. Additionally, by paying attention to your triggers, you gain more control over how your skin feels each day.